Pancreatic duct blockage: what it is and what to do
A pancreatic duct blockage means the duct that carries enzymes from your pancreas to your small intestine is narrowed or closed. That stop causes enzyme backup, pain, inflammation, and trouble digesting fats. You can get a blockage suddenly or over time. Causes range from gallstones and strictures after inflammation to tumors that press on the duct.
How will you notice it? Sharp upper belly pain that radiates to the back is common. Nausea, vomiting, oily stools (steatorrhea), unexplained weight loss, and jaundice (yellow skin or eyes) are red flags. If the duct is blocked long enough you may also develop diabetes because the pancreas cannot make or release insulin properly.
Tests doctors use
Start with blood work for amylase, lipase, liver tests, and bilirubin. A transabdominal ultrasound often finds gallstones and bile duct dilation. CT scan shows inflammation, fluid collections, and tumors. MRCP (magnetic resonance cholangiopancreatography) maps the ducts noninvasively. ERCP (endoscopic retrograde cholangiopancreatography) is both diagnostic and therapeutic — doctors can see the narrowing and place stents or remove stones during the same procedure.
Common treatments and what to expect
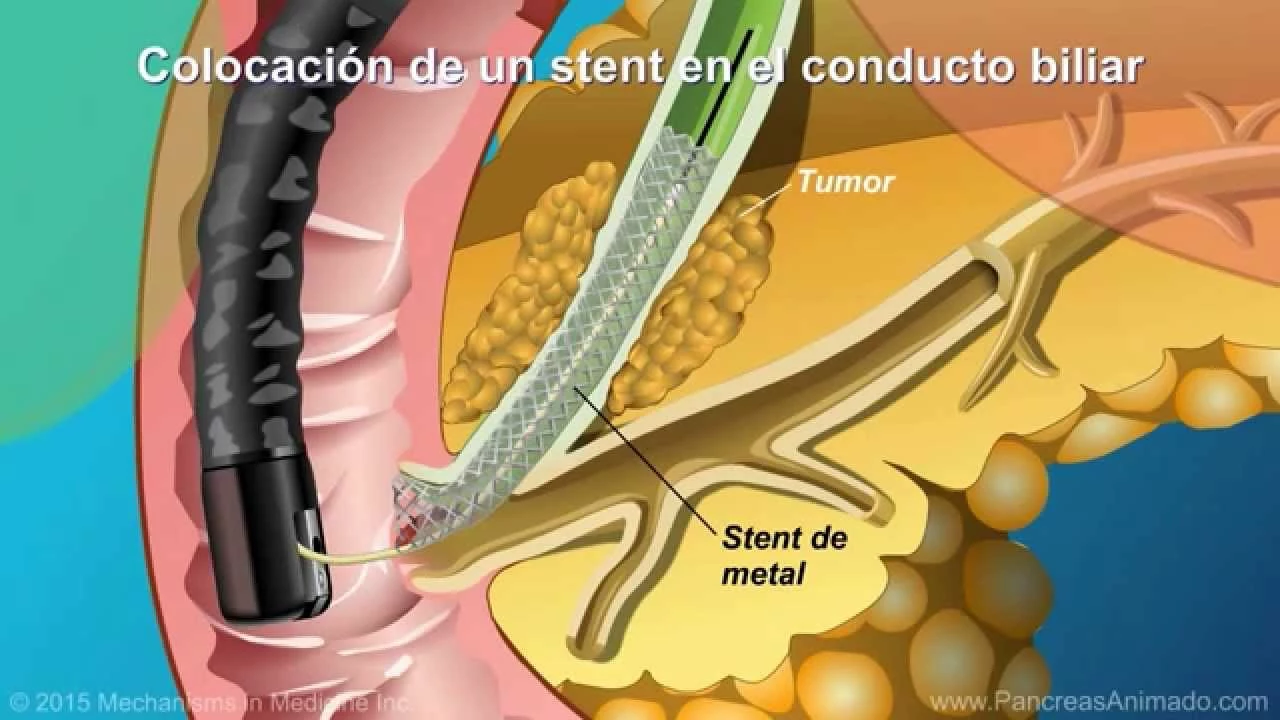
If a gallstone blocks the duct, doctors usually remove it with ERCP. For strictures or persistent narrowing, an ERCP-guided stent can keep the duct open for weeks to months. Some strictures need repeated stent changes or surgery to remove scarred sections. Tumors that cause blockage may require surgery, chemotherapy, or radiation depending on the type and stage.
Infected obstructions (cholangitis or infected pancreatic collections) are medical emergencies. You may need IV antibiotics, urgent drainage, or emergency ERCP. For chronic problems, pancreatic enzyme replacement helps digestion, and fat-soluble vitamin supplements may be needed. Pain control and nutrition support are key while healing happens.
Can you prevent a blockage? You can reduce some risks. Treat gallstones if they cause symptoms. Limit heavy alcohol use and control triglycerides — both lower risk for recurrent pancreatitis and scarring. If you have recurrent acute pancreatitis, follow your doctor’s plan so scar-related strictures don’t form.
When to seek care: go to the ER for severe belly pain, fever with jaundice, fainting, or fast heartbeat. Call your doctor if you have ongoing dull pain, weight loss, new jaundice, or greasy stools. Early testing and treatment lower the chance of complications like chronic pancreatitis, infections, or pancreatic failure.
Questions to ask your doctor: What caused the blockage? Do I need ERCP now? Will I need a stent or surgery? How will we manage pain and digestion after treatment? Clear answers help you make safer choices and plan recovery.
Follow-up after treatment matters. Expect one or more imaging tests to check stent position or duct healing. If you have enzyme replacement, track stool changes and weight. Report persistent pain, fevers, or signs of infection right away. Ask for a clear plan about stent removal timing and when to return for repeat ERCP. Keeping a simple symptom diary makes clinic visits more useful and helps doctors spot problems early.
The Role of Naturopathic Medicine in Treating Pancreatic Duct Blockage
In today's blog post, we explored the role of naturopathic medicine in treating pancreatic duct blockage. We discussed how naturopathic approaches, such as dietary changes, herbal remedies, and stress management, can help address the root causes of the blockage and support overall pancreatic health. We also highlighted the importance of working closely with a qualified naturopathic practitioner to develop a personalized treatment plan. Additionally, we emphasized the need for proper diagnosis and collaboration with conventional medical professionals to ensure the best possible outcome. Overall, naturopathic medicine can be a valuable tool in the management of pancreatic duct blockage, offering a holistic and integrative approach to healing.
read more