Diabetes: Practical Care, Meds & Everyday Tips
Diabetes changes daily life, but small, practical steps have big effects. Want simple actions you can start today? This page pulls together easy-to-use advice on monitoring, daily habits, medications, and safety issues you’ll see in our related articles.
Daily checks and habits that actually help
Check blood sugar regularly if your provider recommends it. Use the numbers to learn patterns, not to judge yourself. Try a short log: time, reading, recent food, and how you felt. That helps you and your clinician spot trends faster than memory alone.
Move more in ways you enjoy. Walking 20–30 minutes after a meal can lower post-meal spikes. Aim for consistent activity across the week instead of random intense workouts. Small bursts of movement — a brisk walk, stairs, or a short bike ride — add up.
Focus on real-food portions, not fad diets. Manage carbs with portion control and consistent timing. Include lean protein, vegetables, and healthy fats to slow digestion and blunt sugar surges. If you’re unsure how many carbs to eat, ask a dietitian for a simple plan based on your routine.
Protect your feet. Daily foot checks catch blisters, cuts, or pressure spots before they worsen. Wear supportive shoes, keep nails trimmed, and see a provider sooner if you notice numbness, burning, or a non-healing sore.
Medications, safety checks, and practical red flags
There are several diabetes medicines: metformin, insulin, SGLT2 inhibitors, GLP‑1 receptor agonists, and others. Each works differently and has pros and cons. If a new med is started, ask how it affects blood sugar patterns, weight, kidney function, and whether it interacts with your other drugs.
Tell every clinician about all your medications, including blood thinners like Plavix or Coumadin, diuretics, and over-the-counter supplements. Diabetes often comes with heart or kidney issues, and some drug combinations need dose changes or closer monitoring.
Know the common warning signs: very high or very low blood sugar, sudden vision changes, severe dehydration, or infections that won’t heal. If you get persistent nausea, chest pain, shortness of breath, or confusion, seek care right away.
Sick-day rules matter. When you’re ill, blood sugar and fluid balance change. Keep quick sources of glucose handy for lows, stay hydrated, monitor more often, and call your healthcare team about insulin or pill dosing during illness.
Shopping for medication online? Use trusted pharmacies and verify credentials. Our site focuses on safe-shop practices and accurate drug info — but always confirm prescriptions with your doctor and pharmacist.
Want step-by-step help? Look through our guides on blood thinners, stent care, and medication alternatives if you need extra context for diabetes-related issues. And if something doesn’t feel right, trust your instincts and reach out to a clinician. Small, steady steps are the most reliable path to safer, clearer diabetes care.
Diabetes and Congestive Heart Failure: How They’re Linked
Explore how diabetes fuels congestive heart failure, the shared risk factors, treatment overlap, and latest research to help patients and clinicians manage both conditions effectively.
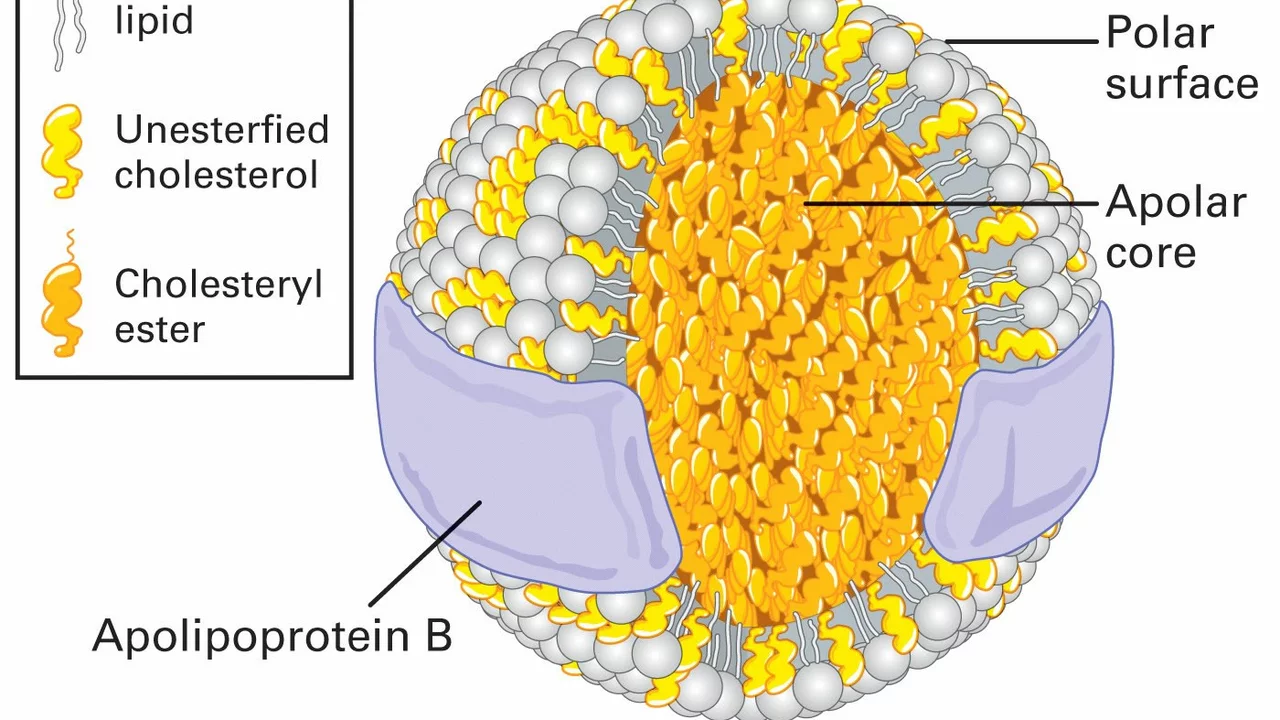
read moreThe Role of Low-Density Lipoprotein in Diabetes
Alright folks, let's tackle this beast of a topic, the role of our not-so-favorite Low-Density Lipoprotein (LDL) in the wide world of diabetes. Now, LDL is often dubbed the 'bad cholesterol' and boy, it lives up to its name in our diabetes story. It struts around our bloodstream, depositing cholesterol on our artery walls and making things a bit too crowded in there. When it comes to diabetes, our dear LDL is a double whammy, not only contributing to heart disease but also making diabetes management harder. So, remember folks, while LDL might be the life of the party in your bloodstream, it's definitely one guest we could do without in the diabetes ball!
read more