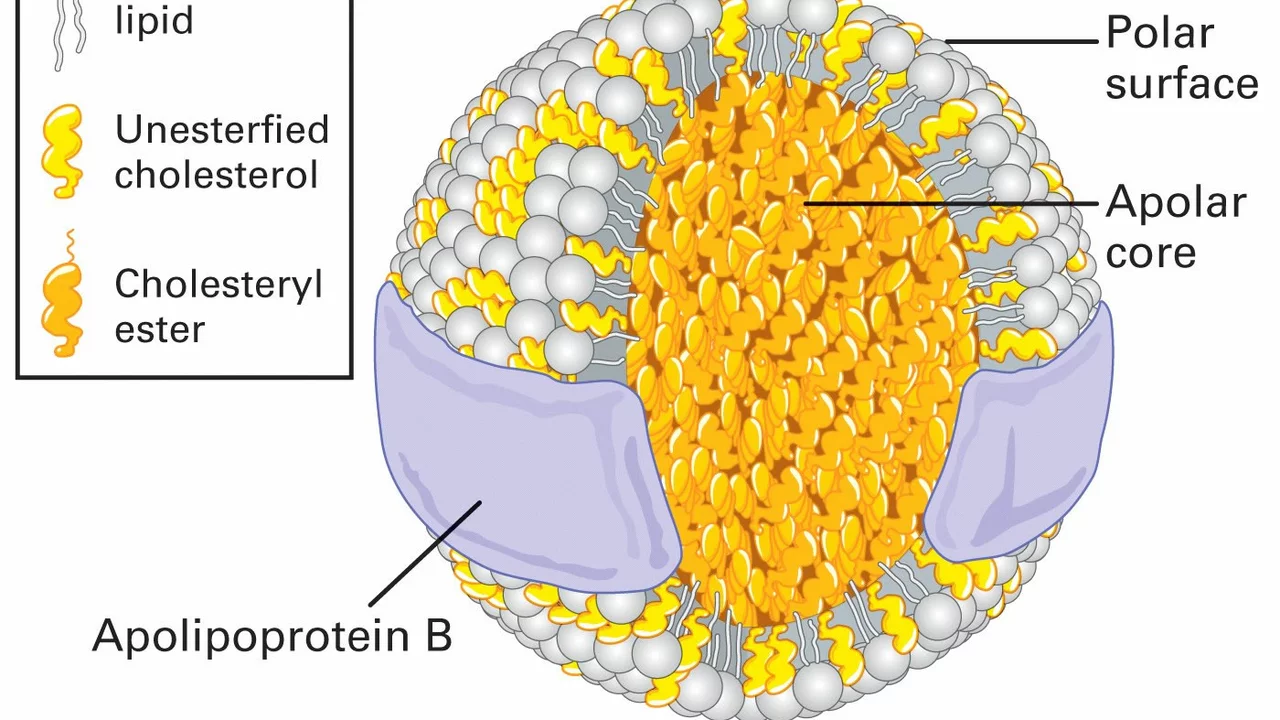
Low-density lipoprotein (LDL): what it means and what to do
LDL is often called the “bad” cholesterol because it carries cholesterol into your artery walls and fuels plaque. High LDL raises your risk of heart attack, stroke, and complications after procedures like stent placement. The good news: lowering LDL clearly reduces those risks and there are simple, proven steps you can take.
How LDL is measured and what the numbers mean
Your cholesterol blood test reports total cholesterol, HDL, triglycerides, and usually LDL. Targets most doctors use: below 100 mg/dL is desirable, under 70 mg/dL for people at very high risk (like those who've had a heart attack), 100–129 is near-optimal, 130–159 borderline high, 160–189 high, and 190+ very high. Labs often calculate LDL with a formula (Friedewald); if your triglycerides are very high (>400 mg/dL) that calculation can be wrong, so your doctor may order a direct LDL or advanced testing.
Practical steps that actually lower LDL
Start with the basics that work for most people: diet, movement, weight, and smoking. Small changes add up.
Diet: cut saturated and trans fats (think fatty cuts of meat, butter, margarine, and many packaged snacks). Swap in healthy fats like olive oil and avocado. Add soluble fiber—oats, beans, lentils, apples, and pears—because it binds cholesterol and helps remove it. Consider plant sterols or stanols (found in some fortified spreads and foods) to lower LDL by a measurable amount. Limit sugary drinks and highly processed foods.
Exercise and weight: aim for 150 minutes of moderate activity a week (brisk walking, cycling). Losing even 5–10% of body weight lowers LDL and improves overall heart risk.
Medications: statins are the first-line drugs to lower LDL and reduce heart events. If statins aren’t enough or aren’t tolerated, doctors may add ezetimibe or newer options like PCSK9 inhibitors. Discuss benefits and side effects with your clinician—drug choice depends on your personal risk and other medicines you take.
Other practical tips: stop smoking, limit alcohol, and control blood pressure and diabetes—these all change how harmful LDL is in your arteries.
If you’ve had a stent or take blood thinners (articles on our site like “Coumadin” and “Plavix” explain those meds), managing LDL is even more important. High LDL speeds plaque build-up and raises the chance of future problems around stents.
Want a simple next step? Check your latest cholesterol numbers, write them down, and talk to your doctor about target LDL for your situation. If you don’t have numbers yet, ask for a fasting or non-fasting lipid panel—either can work for most people—and bring the results back so you can make a clear plan.
If you want practical reads next, search our site for posts on blood thinners, stent care, and cholesterol-lowering options to see how LDL fits into the bigger picture of heart health.
Low‑Density Lipoprotein Myths Debunked: Facts You Need
A clear, fact‑based guide that busts the most common myths about low‑density lipoprotein, explains its role, and shows how to interpret cholesterol results for heart‑health decisions.
read moreThe Role of Low-Density Lipoprotein in Diabetes
Alright folks, let's tackle this beast of a topic, the role of our not-so-favorite Low-Density Lipoprotein (LDL) in the wide world of diabetes. Now, LDL is often dubbed the 'bad cholesterol' and boy, it lives up to its name in our diabetes story. It struts around our bloodstream, depositing cholesterol on our artery walls and making things a bit too crowded in there. When it comes to diabetes, our dear LDL is a double whammy, not only contributing to heart disease but also making diabetes management harder. So, remember folks, while LDL might be the life of the party in your bloodstream, it's definitely one guest we could do without in the diabetes ball!
read more